The night her baby’s heart stopped, Clare* blamed herself. Had she taken her out in the cold too much? Had she damaged her lungs by drinking iced water when she was pregnant? She fixated on Andi’s tiny chest, willing it to suck in air, rushing her to hospital in Fiji for the second time in as many days.
All through the early hours Andi* clung to life. Doctors performed CPR several times, puncturing the month-old baby’s chest to insert a drain, removing fluid from around her lungs. “She was really, really sick and they didn’t know what was going on … she was getting weaker and weaker,” Clare says. She sat by her daughter’s bedside. She prayed.
Then, doctors asked to do an HIV test. Clare was confused, telling doctors she didn’t have it. She’d already taken a test.

No, we mean for the baby, doctors told her.
Andi was HIV positive. So were Clare and her husband. During late pregnancy or while breastfeeding, Clare had contracted the virus and passed it to her daughter, who will now live the rest of her life with a chronic disease. “I thought it was the end of the world,” Clare, who is in her early twenties, says. She turned to her husband, an injecting drug user. “He said, ‘No, I’ve been cautious with this.’ I said, ‘I don’t know. We don’t know. So we’ll just have to figure this out, for the betterment of her’.”
Clare’s young family is one of thousands caught up in Fiji’s HIV crisis, with new cases more than tripling between 2023 and 2024. More than 1,200 people were diagnosed in the first six months of 2025 alone, the world’s fastest-growing HIV epidemic amid a decline in global aid. The UN says Fiji’s location as a drug-running hub and escalating local methamphetamine use has fuelled the rapid spread, coupled with unsafe injecting practices and lack of access to clean needles. Low health awareness, cultural stigma and inadequate testing and treatment have exacerbated the crisis.
It has become a disease of the young and addicted, with half of those who contract HIV thought to have done so through contaminated needle sharing or drug preparation. Now, infections are growing among the most vulnerable: the wave of babies who are being born with – and dying from – complications due to HIV or Aids.
The health authorities told the Guardian that one baby a week is being diagnosed with HIV from mother-to-child transmission, with intensive care units seeing an influx of babies needing life support. One child under the age of five is dying every month, says Dr Jason Mitchell, the head of Fiji’s HIV epidemic response, as doctors frantically try to figure out what is wrong with them.
“It is the figure that I feel most pained by, because it is preventable,” he says. “It is inexcusable to have any more children born with HIV.”

At the edges of this crisis, however, there is some hope. Doctors are among those teaching others that with treatment, comes life; that it is better to seek help than die of Aids, despite the enduring stigma.
‘I’ve seen walking skeletons’
Fiji, an archipelago in the South Pacific Ocean known for its tropical reefs and beaches, has a population of about 930,000. It is a deeply Christian country made up of more than 300 islands, where religion coexists with traditional beliefs. Customary healing and a distrust of western medicine is still commonplace among the iTaukei, or Indigenous Fijians, who make up roughly half of the population. iTaukei are more likely to live in poverty, and make up about 90% of those diagnosed with HIV.
“If you’re living with HIV you’re sinful, you’re going to hell, period. Because we’ve been grounded in religious values, that whatever the preacher says about ‘HIV is a sin’ it is seeded in our heart,” says Christopher Lutukivuya, 38, an HIV activist who has been living with the condition since 2013.

He has seen friends turfed out of family homes or made to live in basements, and those who prefer to deny they are sick or take their own lives rather than admit they have HIV. He picks up medication for those who do not want to be seen in clinics, and drives people to get tested.
“One of the problems we have right now is acceptance. It’s a major issue. I’ve seen walking skeletons, of not wanting to go to the hospital, which has broken my heart.”
Those in Fiji working for the World Health Organization (WHO) and UNAids, the UN agency that fights HIV and Aids globally, say the most basic knowledge around HIV is severely lacking.

“The sorts of things that were issues in Australia in the 1980s, we’re now seeing in the Pacific,” says Dr Mark Jacobs, the WHO representative for the South Pacific. This includes not knowing about the dangers of sharing needles, the lack of a safe needle programme – which is now being set up by Fiji’s Ministry of Health – knowledge of treatment, and acceptance of condom use.
“It’s a degree of naivety, but also because the way the infection is spread can be quite uncomfortable for many people to even think about.”
In villages, some leaders spoken to by the Guardian did not know that HIV could be passed from mothers to babies, or said this was the mother’s fault. Many did not know that HIV was treatable – a misconception in cities, too.
“I thought it was a death sentence,” says Francine*, an Indo-Fijian woman in her mid-30s who found out she had contracted HIV from an IV-drug-using partner when she was breastfeeding. She would have liked to have used a condom, but says she couldn’t ask.
“I’m educated, I know about it, but I can’t negotiate condom use with my partners,” she says. “The power dynamics in Fiji, you cannot.”
Young and addicted
On the streets of Fiji’s capital Suva, the air is warm, but the nights are fraught. Kids survive here by mugging or being used as drug pushers. Many of them inject the first time they encounter meth; it’s quicker and cheaper, and more of them can get high at once.
“Most of the children that we speak with prefer staying on the streets because this is where they get the drugs,” Dr Dashika Balak says. “They are among their friends, and this is where they find what they call love.”
Children become addicted to meth as it flows through Fiji on the way to New Zealand and Australia, with transnational criminal syndicates now also targeting Fiji as a market.
At the Kauwai Youth Restoration Home, social workers led by the pastor Amani Waqetia work to rehabilitate young people, showing them what life without drugs and fear looks like. Among the young people living here are Isac*, 17, who ran away from an abusive uncle, and Nemaia*, 15, who fell in with the wrong crowd. They both became addicted to meth and contracted HIV through needle sharing.
Isac, moving draughts around on a board game at the boys’ home in Suva, says: “I was fit. And after that, I became slim. I lost all my weight. I got it in my body … when we share needles, the bacteria for that person will come to me.”.

“I knew that the drugs are bad for my health. I just keep on doing.” He beat the habit, with social workers – many of whom used to live on the streets themselves – focusing on his diet, structured routine, talk therapy, and reintroducing him to society and faith. Now, he is back at school, enjoys playing guitar, and wants to be an accountant. He’s a good sprinter and trains now for athletics. “I just want to change my life, become a better person. Achieve my goals.”
Nemaia, who spent two years stealing and scavenging on the street, was brought to the hostel by social welfare after a video in which he shot up another boy using a needle went viral on social media. Sitting beside him now, the pride in social worker Maika Barinisavu’s voice is evident when he says how much Nemaia, once wide-eyed and aggressive, has improved; he’s healthy, at peace, and considered one of the leaders. Finding out he had HIV was scary, Nemaia says, but his daily medication means he can live a normal life,and that’s what he tells the new boys who come in here. “I thought I was going to heaven. I was walking up there. Now I’m feeling fresh.”

‘People affected are completely innocent’
Telling a child they have HIV is a learned skill. Most of them don’t understand, even as their parents cry beside them.
“Developmentally, they still don’t really get it,” says Dr Kesaia Tuidraki, the chief medical officer at the sexual and reproductive health clinic Medical Services Pacific.
On average, one person with HIV will spread it to ten others, she says – mostly through shared needles. Transmission also occurs through unsafe sex, and rape. Dr Tuidraki routinely gives HIV prophylaxis to rape and sexual assault victims, effective within 72 hours of the assault. Most cases are girls under the age of 18 and can include several members of the same family. “It’s hard to stomach when the people who are impacted by this are completely innocent,” she says.
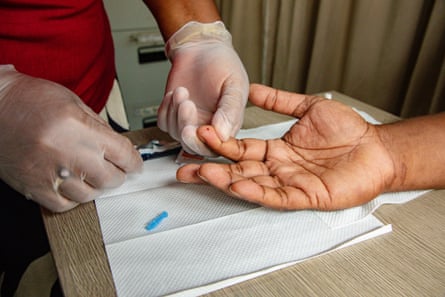
But through Tuidraki’s work, and the work of others, some small shifts are happening. Her organisation has ramped up testing, taking mobile clinics to the streets of Suva and into remote villages.
If HIV is detected in early pregnancy, antiretroviral medications can be started so that the disease can become virally suppressed, lowering or completely preventing the risk of transmission from mother to child.
Renata Ram, an adviser on the Pacific to UNAids, says along with introducing more antenatal testing and earlier maternity care, it was working with the Fiji government on making Prep – pre-exposure prophylaxis – available in the next six months through tablets, injectables, and a vaginal ring that women can wear in secret.
“Most women that are being picked up right now are not injecting drug users, not sex workers. The majority of them are married women who get HIV within their marriage and who do not have much say in terms of their protection,” she says.
Ram says the aim of the HIV program is to “reduce harm while we are still working on the human rights aspect of things. These cultural changes take generations, so we are giving women a choice to protect themselves.”

After seven months on life support, Andi is a happy two-year-old, a scar on her left ribcage the only clue to the night Clare almost lost her. She takes her lifelong anti-retroviral meds crushed up in juice. But Clare watches her closely; despite being careful, Andi has been in and out of hospital, the last time two weeks ago. “If you want your child to be alive, you just have to follow what they say.”
The authorities are expected to upgrade the pandemic threat level to that of a generalised epidemic in the coming months – and while the Fijian government pumped $10m last year into the response, an amount matched by millions in support from Australia and New Zealand, more pressure is needed, Mitchell says. “It cannot just be business as usual.”
‘You can write a new chapter’
Up to 8,900 people are living with HIV in Fiji, according to data from UNAids, a number authorities admit may not reflect the full picture. The 126 official deaths recorded in 2024 are also not considered a representative figure as Mitchell and others tell the Guardian that often in Fiji even when a death is thought to be linked to HIV or Aids, that will not be recorded to avoid bringing shame on patients or their family.

In Fiji’s villages, leaders are in no doubt as to what is in store for them all if HIV continues to spread. As the sun sets on a kava ceremony in Nataleira, a village south of Suva, elders talk about the threat; they want to be prepared, to get tested. “I don’t want one of my family members to be affected because that [virus] kills a generation,” says Rusiate Togotogorua, the headteacher of 170 kids at Navunisaa district school. “Not just one, but a generation. It will come.”
Not all those in villages like to talk. Some expel those with HIV, but places where those people can be cared for are springing up, too.
On the outskirts of Nadi, down the end of a long, rutted driveway in the countryside, a group of women laugh, ribbing each other. They are on their way to a safe house which caters mainly for women, trans women and children who are survivors of drugs, HIV, sexual and domestic violence. On a Monday night in February, there are 68 people there, including 13 kids, and hundreds have been through since it opened in 2019.

“This issue is related to everybody,” says Edwina Biyau, a trans woman and former sex worker who founded the Daulomani Safe House after seeing the need for more prevention and support for those living with HIV.
“You can say that you’re innocent. You’re not going out. You’re just going to church. But how about your husband? How about your uncle? How about your brother? How about your children? We get frustrated because everyone doesn’t want to be part of it, you know. ‘Oh, that’s for sex workers. That’s for drug addicts.’ But that’s why so many people are dying. Because it’s too late.”
When people Biyau suspects have HIV come in, she presents them with Josy Ralulu. A giggly, glowing picture of health, Ralulu is a sex worker who found out she had HIV in 2022 after Biyau urged her to get tested when she had symptoms of what she thought was syphilis.
“At first, I was shocked,” Ralulu says. “I thought I was dead. And then the doctor told me, calm down. There’s medication for it that’s gonna make you live.”

For Biyau, who the girls here call mother, the only way forward is with love, and with hope. In a culture that’s so close-knit, it’s the only thing she sees working.
“You got infected with HIV. But that’s not the end of the world. You know, you can write a new chapter. You can have a new story to tell. This is what happened, and this is hope. You still can live.”
*Names have been changed

.png) 2 months ago
67
2 months ago
67